Several genes in our bodies have been linked -- to varying degrees -- to our chance of developing preeclampsia. A gene is a region of your DNA that holds the instruction manual for making proteins that are the building blocks of most of life's functions. The MTHFR gene provides the instructions to make an enzyme called methylenetetrahydrofolate reductace (try saying that fast!). This enzyme helps to process amino acids that are the building blocks of proteins.
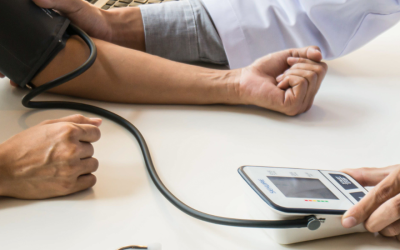
Studies have shown that variations, or subtle differences, in the MTHFR gene are associated with increased risk for many common conditions including heart disease, stroke, high blood pressure, and preeclampsia, among several others. MTHFR helps metabolize folic acid that leads to the breakdown of an amino acid homocysteine. Homocysteine is increased with heart disease, stroke, high blood pressure, and preeclampsia. One variant of the gene for MTHFR is very common and makes a "weak enzyme" that doesn't work as well. It's thought that the weak enzyme leads to an increase in homocysteine, which explains why this gene variant is associated with cardiovascular disease and preeclampsia.
What does this have to do with preeclampsia?
Homocysteine is increased in preeclampsia and MTHFR mutations are more common in preeclampsia. However, it appears that the weak enzyme, if supplied with more folic acid (the amount available in prenatal vitamins), will work well enough to prevent higher homocysteine in normal pregnant women. Higher homocysteine is still present in women with preeclampsia but is not related to whether the woman has the abnormal gene or not.
What do we need to learn?
Despite the ability of folic acid to protect against high homocysteine, which is thought to be why the MTHFR gene variant is associated with preeclampsia, reports of an association of the abnormal gene and preeclampsia persist. This may be related to the vulnerable population not taking folic acid or there may be another effect of the abnormal gene.
What should you do with this information?
There are a few things to consider before running out and getting tested for variations in the MTHFR gene. First, there is the very real possibility that folic acid can reduce the risk. Second, the effect of MTHFR to increase the risk of preeclampsia is small. In analyses of available studies, the increased risk is 20 percent to 30 percent (compared to 300 percent with obesity). Talk to your doctor about the benefits and disadvantages of genetic testing. Discuss what you would do with the results and if they could potentially change any current treatment plans or affect future decisions. And be sure to take prenatal vitamins with at least 400 micrograms of folic acid if you are pregnant or planning to become pregnant.
Genetic testing can be costly and may not be covered by your insurance. Contact genetics labs to obtain their rates and check with your insurance to make sure you know ahead of time about any out-of-pocket costs.
Finally, every year scientists are learning and developing more efficient ways to study genetics and develop clinical tests. The Preeclampsia Foundation is dedicated to being at the forefront of preeclampsia research to bring you the most up-to-date information on scientific advances and breakthroughs.
Sources:
1. Ubeda N, Reyes L, Gonzalez-Medina A, Alonso-Aperte E and Varela-Moreiras G. Physiologic changes in homocysteine metabolism in pregnancy: A longitudinal study in Spain. Nutrition. 2011;27:925-930.
2. Powers RW, Dunbar MS, Gallaher MJ and Roberts JM. The 677 C-T methylenetetrahydrofolate reductase mutation does not predict increased maternal homocysteine during pregnancy.Obstetrics & Gynecology. 2003;101:762-6.
3. Yang BY, Fan SJ, Zhi XY, Li YF, Liu YY, Wang D, He M, Hou YY, Zheng QM and Sun GF. Associations of MTHFR Gene Polymorphisms with Hypertension and Hypertension in Pregnancy: A Meta-Analysis from 114 Studies with 15411 Cases and 21970 Controls. PlosOne. 2014;9.
4. Wang XM, Wu HY and Qiu XJ.Methylenetetrahydrofolate Reductase (MTHFR) Gene C677T Polymorphism and Risk of Preeclampsia: An Updated Meta-analysis Based on 51 Studies. ArchMed Res. 2013;44:159-168.
Special thanks to Dr. James Robert, Co-chair of The Preeclampsia Registry Advisory Council and member of the Preeclampsia Foundation's Medical Advisory Board, for his editorial assistance with this Ask an Expert article.






1777566412.png)
1777563523.png)
1777562643.png)